Hormonal acne is a common skin condition triggered by fluctuations in hormones, particularly androgens, which stimulate the sebaceous glands to produce excess oil. This often results in painful, deep-seated cystic breakouts typically concentrated along the lower face and jawline. Unlike standard surface pimples, it is biologically driven and requires targeted internal or external medical intervention.
What Is Hormonal Acne?
How Hormonal Acne Develops
Hormonal acne begins deep within the pores when an increase in androgen levels signals the sebaceous glands to overproduce sebum (natural oil).
This excess oil mixes with dead skin cells, creating a plug that traps bacteria, specifically Cutibacterium acnes, leading to inflammation.
Because the trigger is systemic (internal), the inflammation is often more severe and deeper than common whiteheads.
In the humid Malaysian climate, where the average humidity is around 80%, this oil production can become even more aggressive, leading to persistent congestion.
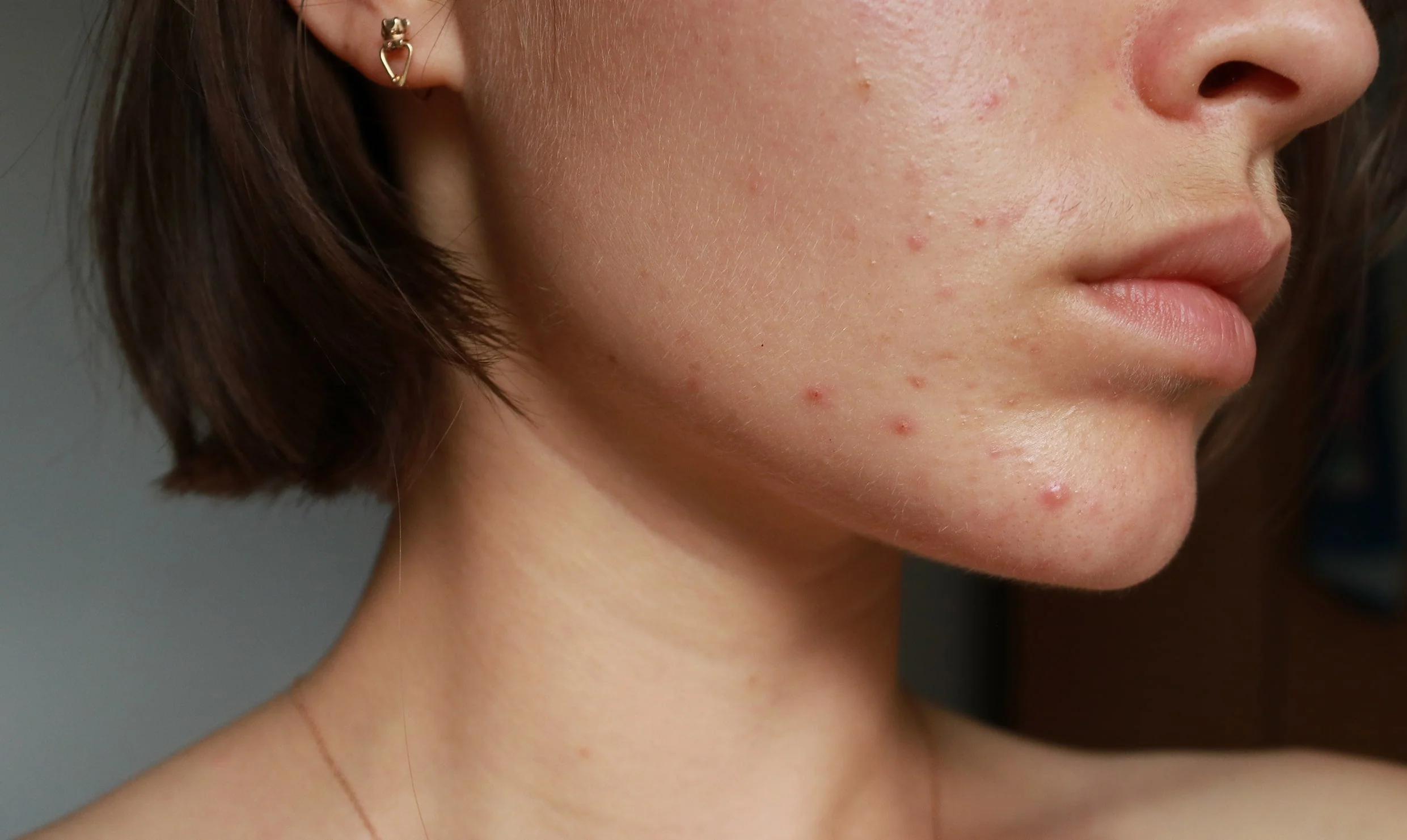
Common Areas Affected (Jawline, Chin, Lower Face)
One of the most telling signs of this condition is its “U-zone” distribution, primarily affecting the chin and jawline.
While teenage acne often appears in the T-zone (forehead and nose), adult hormonal breakouts favor the lower third of the face.
Some individuals may also experience breakouts on the neck, shoulders, or back during significant hormonal shifts.
This specific mapping helps Ministry of Health (MOH) certified dermatologists differentiate between lifestyle-induced skin irritation and true hormonal imbalances.
What Causes Hormonal Acne?
Androgens and Excess Sebum Production
Androgens, such as testosterone, are the primary drivers of sebum production in both men and women.
When these hormone levels spike, the skin’s oil becomes thicker and more abundant, making it significantly harder for pores to remain clear.
This process is a biological chain reaction that cannot be fixed by washing your face more frequently; it requires balancing the skin’s environment.
Menstrual Cycle, PCOS, and Hormonal Fluctuations
For many women, breakouts peak during the week before menstruation when estrogen levels drop and progesterone rises.
Conditions like Polycystic Ovary Syndrome (PCOS) can cause chronic hormonal acne due to elevated androgen levels and insulin resistance.
Other life stages, such as pregnancy, postpartum, and perimenopause, are also major triggers for these persistent skin changes.
Research suggests that hormonal acne and PCOS are frequently linked, often requiring a multidisciplinary approach involving both a gynecologist and a skin specialist.
Stress and Lifestyle Triggers
High stress levels trigger the adrenal glands to release cortisol, which indirectly boosts oil production and worsens inflammation.
Diets high in refined sugars and high-glycemic index foods (like white rice and sugary local desserts) can spike insulin, further stimulating androgens.
Lack of sleep disrupts the body’s natural circadian rhythm, preventing the skin from entering its essential repair and detoxification mode at night.
Signs of Hormonal Acne
Cystic and Deep Inflammatory Acne
Unlike small surface bumps, hormonal acne often manifests as cysts—large, red, and painful lumps that never come to a “head.”
These lesions stay deep under the skin for weeks and are much more likely to leave behind permanent atrophic acne scars if not treated correctly.
Because they are inflammatory, they often feel warm to the touch and can cause a throbbing sensation.
Recurring Breakouts in the Same Area
A hallmark sign is the “phantom” pimple—a breakout that clears up only to reappear in the exact same pore or spot a month later.
This happens because the underlying inflammation in that specific follicle remains dormant until the next hormonal surge triggers it.
This repetitive cycle is a clear indicator that topical surface treatments alone are insufficient for long-term clearance.
How to Identify Hormonal Acne
If your breakouts correlate with your monthly cycle or periods of intense stress, it is likely hormonal in nature.
You can identify it by the texture (hard, deep lumps) and the location (concentrated on the lower face).
If you are over the age of 25 and suddenly experiencing “teenage-style” breakouts, it is almost certainly adult hormonal acne.
How to Treat Hormonal Acne
Medical Treatments (Hormonal Therapy, Oral Medications)
For severe cases, doctors may prescribe oral contraceptives (birth control pills) to regulate the estrogen-progesterone balance.
Spironolactone, originally a blood pressure med, is often used “off-label” to block the effects of androgens on the sebaceous glands.
In persistent cases where scarring is a high risk, Oral Isotretinoin may be recommended to permanently shrink oil glands, though this requires strict medical supervision.
Topical Treatments for Hormonal Acne
Topical Retinoids (like Tretinoin or Adapalene) are the gold standard for keeping pores clear and speeding up cellular turnover.
Benzoyl Peroxide is effective for killing acne-causing bacteria, though it should be used in lower concentrations (2.5%) to avoid excessive dryness.
Azelaic Acid is an excellent alternative for those with sensitive skin, as it reduces both inflammation and the dark spots (PIH) left behind by cysts.
Skincare Routine for Acne Control
Use a gentle, pH-balanced cleanser twice daily to remove pollutants without stripping the skin’s protective barrier.
Incorporate a non-comedogenic (oil-free) moisturizer to prevent the skin from overcompensating for dryness by producing more oil.
Always finish with a broad-spectrum sunscreen of at least SPF 30 or higher, as many acne treatments increase sun sensitivity.
Aesthetic Treatments for Hormonal Acne in Malaysia
Laser Treatments and Light Therapy
Pico Laser and Dual Yellow Laser are popular in Malaysia for reducing the redness and bacterial load associated with active acne.
These lasers work by targeting the blood vessels feeding the inflammation and stimulating deep collagen to prevent future scarring.
Treatments are typically quick, with sessions lasting 15 to 20 minutes and involving minimal downtime.
Chemical Peels and Acne Facials
Medical-grade Chemical Peels (using Salicylic or Glycolic acid) help exfoliate the skin deeply and unclog congested pores.
Prices for superficial peels in local clinics usually start from RM200 to RM450 per session, depending on the acid concentration.
Professional acne facials focus on safe extractions to remove “plugs” before they turn into inflamed cysts.
Acne Injections for Severe Cases
For emergency “big event” breakouts, a doctor can administer a corticosteroid injection directly into the cyst.
This reduces inflammation within 24 to 48 hours, preventing the cyst from rupturing and causing a deep scar.
It is a quick, localized treatment that provides immediate relief from the pain and pressure of a large cyst.
Best Ingredients for Hormonal Acne
Salicylic Acid, Retinoids, Niacinamide
Salicylic Acid (BHA): An oil-soluble acid that dives deep into the pores to dissolve the “glue” holding dead skin cells together.
Retinoids: These vitamin A derivatives are the “heavy lifters” that remodel the skin and prevent the formation of comedones.
Niacinamide (Vitamin B3): A multi-tasker that regulates oil production, calms redness, and strengthens the skin’s moisture barrier.
Using products with proven acne-fighting ingredients ensures your routine is backed by science rather than marketing hype.
Hormonal Acne Results and Recovery
When Results Start to Show
Because skin cells take about 28 to 45 days to renew, you should expect to see initial improvements after 4 to 6 weeks.
Significant reduction in deep cysts usually occurs after 3 months of consistent medical and topical treatment.
Patience is key; rushing the process with too many harsh products can lead to a compromised skin barrier and more breakouts.
Maintenance and Prevention
Once the skin is clear, a “maintenance” dose of retinoids or periodic aesthetic treatments is often needed to keep pores refined.
Managing stress through exercise and adequate sleep (7–8 hours) is vital to keep cortisol levels from spiking.
Consistent sun protection is mandatory to ensure that the red or brown marks left by acne don’t become permanent pigmentation.
Cost of Hormonal Acne Treatment in Malaysia
Average Price Range
| Treatment Type | Estimated Cost (Per Session) |
| Consultation Fee | RM100 – RM300 |
| Chemical Peel | RM200 – RM450 |
| Pico / Pro-Yellow Laser | RM600 – RM1,500 |
| Oral Medications (Monthly) | RM150 – RM400 |
Factors Affecting Cost
Clinic Accreditation: Clinics with LCP-certified (Letter of Credentialing and Privileging) doctors often have higher safety standards and pricing.
Technology Used: Newer laser models or premium imported chemical peels will generally cost more than basic options.
Geographic Location: Prices in the Klang Valley (KL/Selangor) may be slightly higher than in other states due to overhead costs.
Hormonal Acne FAQs
What causes hormonal acne?
It is primarily caused by an imbalance in androgens which overstimulates oil glands, combined with factors like stress, diet, and genetics.
How do I know if my acne is hormonal?
If your breakouts are deep, painful, and concentrated on your chin and jawline—especially if they fluctuate with your period—it’s likely hormonal.
What is the best treatment for hormonal acne in Malaysia?
A combination of oral medications (like spironolactone or birth control), prescription retinoids, and laser therapy is generally the most effective.
Can hormonal acne be cured permanently?
While it can be managed into complete remission for years, it can occasionally resurface during major life changes like pregnancy or menopause.
How long does hormonal acne take to clear?
Most patients see a noticeable difference in 6 to 12 weeks, with full clearance usually achieved within 3 to 6 months of consistent care.
What is the best skincare for hormonal acne?
A routine featuring a gentle cleanser, a retinoid for cell turnover, niacinamide for oil control, and a non-clogging sunscreen is ideal.
