Safe and Effective Cellulite Treatment in Malaysia for Smoother Skin
Cellulite treatment is a set of non-surgical medical procedures that reduce dimpled skin by breaking down subcutaneous fat, releasing fibrous septae bands, and stimulating collagen production. Common modalities include radiofrequency, acoustic wave therapy, injectable enzymes, and subcision. These treatments improve skin texture, firmness, and body contour without significant downtime. What Is Cellulite? Cellulite is the orange-peel or cottage-cheese skin texture caused when fat pushes through connective tissue bands beneath your skin. It is harmless, very common, and affects most women regardless of weight or fitness level. What Causes Cellulite Hormones – oestrogen plays a major role Genetics – family history increases risk Poor circulation – reduces skin health Sedentary lifestyle – lack of movement Diet – high fat, salt, and carbs Dehydration – reduces skin elasticity Ageing – collagen loss over time Common Areas Affected by Cellulite Thighs (inner and outer) Buttocks Stomach (lower abdomen) Upper arms Types and Grades of Cellulite Grade Appearance Visibility Grade 1 (Mild) Smooth standing, dimples when pinched Not visible naturally Grade 2 (Moderate) Dimples appear standing Visible without touching Grade 3 (Severe) Deep, raised dimples Very noticeable Cellulite vs Fat Cellulite is a structural problem of connective tissue bands pulling skin down while fat pushes up. Body fat is simply stored energy under the skin. Even thin people can have cellulite. How Does Cellulite Treatment Work? Cellulite treatments use four main actions to improve skin appearance. Fat Reduction and Cellulite Reduction Treatments break down fat cell membranes using heat, sound waves, or injectable enzymes. Your body naturally eliminates these fat cells over several weeks, reducing the bulges that create dimples. Collagen Stimulation for Smoother Skin Heat-based treatments (radiofrequency, laser) trigger new collagen production. Collagen is the protein that makes skin smooth and elastic. More collagen means less visible dimpling. Skin Tightening and Firming Radiofrequency and ultrasound heat deep skin layers, causing immediate collagen contraction. This tightens skin right away and continues improving for months as new collagen forms. Improving Blood Circulation Vacuum therapy and acoustic waves boost blood flow to treated areas. Better circulation removes toxins, reduces fluid retention, and delivers oxygen for healthier skin. Types of Cellulite Treatment in Malaysia Radiofrequency (RF) Cellulite Treatment RF uses electromagnetic waves to heat deep skin layers, melting fat and tightening collagen. Pain level: None (warm sensation) Downtime: Zero Sessions: 6-10 Cost: RM 300 – RM 600 per session Acoustic Wave Therapy for Cellulite Sound waves break down fibrous bands causing dimples while improving blood flow. Pain level: None (tapping sensation) Downtime: Zero Sessions: 6-10 Cost: RM 350 – RM 700 per session Ultrasound Cellulite Treatment High-frequency sound waves target and disrupt fat cells without damaging surrounding tissue. Pain level: None Downtime: Zero Sessions: 6-8 Cost: RM 300 – RM 500 per session Laser Cellulite Treatment Light energy melts fat and stimulates collagen for tighter, smoother skin. Pain level: Mild to none Downtime: 0-1 day Sessions: 1-3 Cost: RM 800 – RM 2,000 per session Vacuum Therapy and Endermologie Suction and rolling massage lift skin, break fibrous bands, and improve lymphatic drainage. Pain level: None (massage-like) Downtime: Zero Sessions: 8-12 Cost: RM 200 – RM 400 per session Subcision Cellulite Treatment A needle inserted under skin cuts fibrous bands, releasing the pulling effect. Pain level: Low (local anaesthesia) Downtime: 1-2 days Sessions: 1-3 Cost: RM 1,500 – RM 3,500 per session Injectable Cellulite Treatments Injections dissolve fat cells (Mesolipo) or break down fibrous tissue (enzyme therapy like PB Serum). Pain level: Mild (tiny pricks) Downtime: 0-2 days Sessions: 3-6 Cost: RM 500 – RM 2,700 per session Best Cellulite Treatment for Different Body Areas Thigh Cellulite Treatment Radiofrequency and acoustic wave therapy work best for thighs. They penetrate deeply enough to reach fat layers and fibrous bands. Injectable treatments also work well for localised thigh fat. Buttocks Cellulite Treatment Subcision is most effective for buttocks because it directly releases deep fibrous bands. Follow with radiofrequency for skin tightening. GLOJAS Specialist Clinic offers combination protocols specifically for buttock cellulite. Stomach Cellulite Treatment Laser and radiofrequency treatments work well on stomach cellulite. Ultrasound is also effective for mild to moderate cases. Multiple sessions are usually needed. Arm Cellulite Treatment Radiofrequency and injectable treatments are best for arms because the skin is thinner. Fewer sessions are typically needed due to smaller treatment areas. Benefits of Cellulite Treatment Smoother Skin Texture Treatments break down the fibrous bands and fat that cause dimples, leaving skin visibly smoother. Firmer and Tighter Skin Collagen stimulation makes skin more elastic and resilient, preventing future cellulite formation. Improved Body Contouring Many treatments reduce localised fat while improving cellulite, creating better body shapes. Non-Surgical Cellulite Reduction Most treatments require no incisions, no anaesthesia, and no hospital stay. You return to normal life immediately. Who Is Suitable for Cellulite Treatment? Mild to Moderate Cellulite Grade 1 and 2 cellulite responds excellently to non-invasive treatments like RF, acoustic wave, and ultrasound. Severe Cellulite Cases Grade 3 requires subcision combined with skin tightening. Multiple treatment modalities produce the best results. Cellulite After Pregnancy Treatment is safe after completing breastfeeding and returning to stable weight. Hormonal changes during pregnancy often trigger cellulite. Cellulite After Weight Loss Significant weight loss leaves loose skin and stubborn cellulite. Skin tightening treatments like RF are especially beneficial here. What to Expect During Cellulite Treatment Consultation and Skin Assessment A doctor examines your cellulite grade, reviews medical history, and recommends specific treatments based on your goals and budget. Preparing for the Treatment Avoid blood-thinning medications (aspirin, ibuprofen, fish oil) for 3-5 days before injectable or subcision treatments. Stay hydrated. During the Treatment Session Most sessions last 30-60 minutes. Non-invasive treatments feel warm or tingly. Injectables involve small pricks after numbing cream. Recovery and Aftercare Zero downtime for most treatments. Temporary redness, swelling, or bruising resolves within days. Avoid saunas and vigorous exercise for 24-48 hours. Before and After Cellulite Treatment Expected Results Gradual improvement over weeks to months. Injectable treatments show results after 2-4 sessions. Subcision gives immediate improvement that continues for 3-6 months. Number of Sessions Needed Treatment Sessions Spacing RF / Acoustic wave / Ultrasound 6-10 Weekly Injectable 3-6 2-4 weeks Subcision 1-3 3 months Laser 1-3 Monthly How Long Results Last Non-invasive results last 6-12 months. Subcision can last 2+ years. Maintenance
Pancut Awal (Ejakulasi Pramatang): Punca, Simptom & Rawatan Berkesan
Pancut awal atau ejakulasi pramatang adalah kondisi di mana lelaki mengalami ejakulasi lebih cepat daripada yang diinginkan, biasanya dalam masa kurang dari 1-3 minit selepas penetrasi. Ia adalah masalah seksual paling biasa pada lelaki di Malaysia. Pancut awal boleh menyebabkan tekanan, rasa malu, dan menjejaskan keyakinan diri serta hubungan dengan pasangan. 1. Apa Itu Pancut Awal? Definisi Pancut Awal Menurut Pakar Menurut Persatuan Perubatan Seks Antarabangsa (ISSM), pancut awal ditakrifkan sebagai: Ejakulasi yang selalu berlaku dalam masa 1 minit selepas penetrasi Ketidakmampuan untuk melambatkan ejakulasi Kesan negatif seperti tekanan, kekecewaan, atau mengelak hubungan intim Pancut Awal Primer vs. Sekunder Jenis Definisi Contoh Primer (Seumur hidup) Masalah sejak hubungan seks pertama Lelaki muda yang tidak pernah mampu bertahan lama Sekunder (Diperoleh) Masalah timbul selepas tempoh fungsi seksual normal Lelaki berusia 40 tahun yang sebelum ini boleh bertahan 10 minit Berapa Minit Dikategorikan Pancut Awal? Masa (selepas penetrasi) Status Kurang 1 minit Pancut awal teruk 1 – 2 minit Pancut awal ringan 2 – 5 minit Sempadan normal Lebih 5 minit Normal Kebanyakan lelaki di Malaysia berasa tidak puas jika kurang dari 5-7 minit, walaupun secara perubatan tidak dikategorikan pancut awal. 2. Tanda dan Gejala Pancut Awal Tidak Boleh Kawal Ejakulasi Tanda utama pancut awal: Ejakulasi berlaku lebih awal daripada kehendak Rasa seperti “terpaksa” atau tidak boleh tahan Tidak boleh melambatkan walaupun sudah mencuba pelbagai teknik Kesan Psikologi: Tekanan dan Kurang Keyakinan Kesan pancut awal bukan hanya fizikal. Ia memberi impak besar kepada emosi lelaki: Rasa malu dan rendah diri Mengelak hubungan intim dengan pasangan Tekanan setiap kali sebelum hubungan Kualiti hubungan merosot Pasangan mungkin rasa tidak puas atau salah faham Clinical Experience Insight: Dalam konsultasi, ramai pesakit lelaki mengakui mereka sudah bertahun-tahun mengalami pancut awal tetapi tidak pernah mendapatkan rawatan kerana malu. Mereka cuba pelbagai produk dari internet tanpa hasil. Apabila doktor terangkan bahawa pancut awal adalah masalah perubatan biasa (seperti darah tinggi), ramai pesakit rasa lega dan lebih terbuka untuk rawatan. Jangan biarkan malu menjejaskan hubungan dan keyakinan diri anda. 3. Punca Pancut Awal Punca pancut awal terbahagi kepada dua kategori utama: psikologi dan fizikal. Punca Psikologi: Tekanan dan Kebimbangan Punca Psikologi Keterangan Tekanan prestasi Takut tidak memuaskan pasangan Kebimbangan seksual Rasa gementar sebelum hubungan intim Trauma masa lalu Pengalaman seksual negatif Tekanan kerja/kewangan Gangguan fokus semasa hubungan Hubungan bermasalah Konflik dengan pasangan Punca Fizikal: Hormon dan Keradangan Prostat Punca fizikal yang jarang diketahui: Hormon tiroid tidak stabil (hipertiroid): Metabolisme tinggi, badan terlalu “laju” Keradangan prostat (prostatitis): Keradangan pada kelenjar prostat Ketidakseimbangan serotonin: Neurotransmitter yang mengawal ejakulasi Sensitiviti zakar tinggi: Saraf di hujung zakar terlalu aktif Faktor Gaya Hidup: Merokok dan Kurang Tidur Gaya hidup harian menyumbang kepada masalah ejakulasi: Faktor Kesan Merokok Rosak saluran darah dan saraf Alkohol berlebihan Gangguan sistem saraf Kurang tidur Tingkatkan kortisol (hormon tekanan) Obesiti Gangguan hormon dan aliran darah Kurang senaman Otot lantai pelvis lemah 4. Cara Mengatasi Pancut Awal Di Rumah Sebelum mendapatkan rawatan perubatan, cuba teknik di rumah ini. Ia selamat, percuma, dan berkesan untuk ramai lelaki. Teknik Mula dan Berhenti (Stop-Start) Langkah-langkah: Mulakan rangsangan (sama ada sendiri atau dengan pasangan) Apabila rasa hampir ejakulasi (tahap 7/10), berhenti segera Tunggu sehingga rasa mahu ejakulasi turun ke tahap 3-4/10 Mulakan semula rangsangan Ulang 3-5 kali sebelum ejakulasi penuh Lakukan 2-3 kali seminggu. Hasil kelihatan selepas 4-6 minggu. Tekanan (Squeeze Technique) Sama seperti teknik mula-berhenti, tetapi dengan tekanan fizikal. Langkah-langkah: Apabila rasa hampir ejakulasi, hentikan rangsangan Tekan hujung zakar (glans) dengan ibu jari dan jari telunjuk Tekan selama 10-30 saat sehingga rasa ingin ejakulasi hilang Lepaskan dan mulakan semula Senaman Kegel Senaman Kegel menguatkan otot pubococcygeus (PC) yang bertanggungjawab mengawal ejakulasi. Cara melakukan: Kenal pasti otot PC: Hentikan aliran air kencing di pertengahan Kontra otot selama 3–5 saat Rehat 3–5 saat Ulang 10–15 kali Lakukan 3 set sehari Hasil: Selepas 6-12 minggu, kawalan ejakulasi lebih baik. Penggunaan Kondom Tebal Kebanyakan kondom standard adalah 0.05-0.07mm. Kondom tebal (0.08-0.10mm) mengurangkan sensitiviti. Pilihan kondom untuk pancut awal: Kondom biasa (kurangkan sensitiviti sedikit) Kondom dengan benzocaine/lidocaine (anestetik ringan) Kondom double (pakai dua lapis) – tetapi risiko pecah Masturbasi Sebelum Hubungan Seks Masturbasi 1-2 jam sebelum hubungan seks mengurangkan “tekanan” ejakulasi. Refraktori selepas ejakulasi membolehkan anda bertahan lebih lama pada pusingan kedua. Tips: Jangan masturbasi terlalu awal (contoh 6 jam sebelum) kerana kesannya mungkin sudah hilang. Alihkan Perhatian dan Kawal Pernafasan Fokus pada sesuatu yang neutral semasa hubungan seks. Teknik pernafasan: Tarik nafas dalam selama 4 saat Tahan 4 saat Hembus perlahan selama 6 saat Ulang untuk mengurangkan keterujaan sistem saraf 5. Rawatan Perubatan Pancut Awal Jika teknik di rumah tidak mencukupi, rawatan perubatan adalah pilihan seterusnya. Semua rawatan ini memerlukan preskripsi doktor. Ubat Oral: Dapoxetine (Priligy) Dapoxetine adalah satu-satunya ubat yang diluluskan khusus untuk pancut awal. Maklumat Keterangan Dos 30mg atau 60mg Waktu makan 1-3 jam sebelum hubungan seks Kekerapan Maksimum 1 pil setiap 24 jam Harga RM30 – RM60 setiap pil Kesan sampingan Loya, pening, sakit kepala (biasa ringan) Kesan: Tambah masa tahan 2-4 kali ganda (contoh dari 30 saat ke 2-3 minit) Krim dan Semburan Anestetik Topikal Krim atau semburan yang mengandungi lidocaine atau prilocaine. Cara penggunaan: Sembur/sapu pada hujung zakar Tunggu 5-10 minit Cuci sebelum penetrasi (supaya tidak mati rasa pasangan) Bertahan 2-3 kali ganda lebih lama Harga: RM50 – RM150 setiap botol (tahan 1-3 bulan) Kelemahan: Boleh menyebabkan kebas pada zakar dan pasangan jika tidak dicuci. Suntikan PRP (P-Shot) PRP adalah platelet dari darah pesakit sendiri yang disuntik ke dalam zakar. Prosedur: Ambil darah pesakit (10-20ml) Pusing dalam mesin untuk asingkan platelet Suntik platelet ke dalam tisu zakar Jadual rawatan: 1-2 sesi awal Sesi ulangan setiap 6-12 bulan Harga: RM1,500 – RM3,000 setiap sesi Kesan: Bertambah sensitiviti kawalan, ereksi lebih kuat, tahan lebih lama dalam 2-4 minggu. Terapi Kaunseling Untuk pancut awal yang berpunca dari faktor psikologi (tekanan prestasi, trauma, kebimbangan), kaunseling seksologi sangat membantu. Apa dilakukan dalam sesi kaunseling: Kenal pasti punca psikologi Teknik pengurusan tekanan Latihan komunikasi dengan pasangan Latihan desensitiviti Bilangan sesi: 4-10 sesi (bergantung kepada keparahan) Harga: RM150 – RM400 setiap sesi 6. Kos Rawatan Pancut Awal di Malaysia Harga Ubat dan Konsultasi Rawatan Kos Konsultasi doktor (swasta) RM80 – RM200 Konsultasi
Ginekomastia: Punca, Simptom, Diagnosis & Rawatan Berkesan
Perasan dada nampak ‘membonjol’ walau dah diet dan gym? Bagi lelaki, ini bukan sekadar lemak. Ia mungkin ginekomastia (Gynecomastia Surgery) — pembesaran tisu kelenjar payudara akibat hormon tak seimbang. Isu ini common di Malaysia tapi ramai malu nak tanya. Jom leraikan satu-satu. Apa Itu Ginekomastia Ginekomastia = pembesaran tisu kelenjar payudara pada lelaki. Bukan lemak, tapi tisu sebenar yang membesar sebab nisbah hormon estrogen lebih tinggi dari testosteron. Boleh jadi sebelah atau kedua-dua belah dada. Boleh berlaku pada bayi baru lahir, remaja akil baligh, dan lelaki dewasa 50+. Punca Ginekomastia Pada Lelaki Dewasa & Remaja Kumpulan Punca Paling Lazim Bayi lelaki Estrogen dari ibu. Hilang sendiri 2-3 minggu lepas lahir Remaja 12-17 tahun Lonjakan hormon akil baligh. 70% remaja alami, 90% pulih dalam 6 bulan – 2 tahun Lelaki dewasa 20-40 Ubat: finasteride, antidepresan, ubat gastrik, steroid anabolik, ubat HIV Steroid gym & prohormone Ganja & alkohol kronik Obesiti – lemak tukar testosteron jadi estrogen Lelaki >50 tahun Testosteron menurun semula jadi, penyakit hati, buah pinggang, tiroid, tumor testis/adrenal Ubat yang sering dikaitkan: Spironolactone, ketoconazole, cimetidine, ubat jantung, ubat kemoterapi. Simptom & Tanda Ginekomastia Bengkak bawah puting – rasa macam ada ‘butang’ atau cakera getah yang boleh digerak Sakit/ sensitif bila disentuh – terutama awal jadi. Lama-lama tak sakit Puting terkeluar atau ‘puffy nipple’ Tak simetri – sebelah lebih besar dari sebelah Kulit tak berlekuk – beza dengan lemak biasa Jumpa doktor segera jika: keluar darah dari puting, ketulan keras tak bergerak, kulit berkedut macam kulit oren. Itu tanda kanser payudara lelaki — jarang tapi wujud. Perbezaan Ginekomastia vs Lemak Dada Biasa Ramai lelaki keliru antara ginekomastia dan pseudogynecomastia iaitu lemak dada. Ciri Ginekomastia Lemak Dada Biasa Punca Tisu kelenjar + hormon Lemak berlebihan, obesiti Rasa bila picit Ada cakera keras bawah puting Lembut, sekata, tiada ketulan Respon pada diet/gym Tak kecut walau dah kurus Kecut bila % lemak badan turun Bentuk Kon/tirus ke depan, puting puffy Leper, jatuh ikut graviti Sakit Boleh sakit/sensitif Tak sakit Test mudah: Baring. Guna ibu jari & jari telunjuk, picit perlahan dari tepi ke arah puting. Kalau rasa cakera getah 2-4cm bawah areola = ginekomastia. Cara Diagnosis Ginekomastia di Malaysia Doktor di klinik/ hospital swasta biasanya buat 4 langkah: Sejarah & pemeriksaan fizikal – tanya ubat, suplemen gym, alkohol. Doktor akan rasa tisu dada. Ujian darah – cek testosteron, estradiol, LH, FSH, fungsi hati, buah pinggang, tiroid. Ultrasound payudara – sahkan ada tisu kelenjar vs lemak. Kos: RM150-RM350. Mammogram – jika umur >40 atau ketulan mencurigakan. Kos: RM200-RM450. Kalau disyaki tumor, doktor akan rujuk ujian hormon lanjut & CT scan. Rawatan Ginekomastia: Ubat vs Pembedahan Jenis Bila Sesuai Nota Penting Pemerhatian Remaja, baru jadi <6 bulan 90% kes remaja hilang sendiri. Pakai compression vest sementara Stop punca Akibat ubat/steroid/alkohol Tukar ubat dengan nasihat doktor. Stop steroid gym. Boleh kecut 3-6 bulan Ubat hormon Kes awal <1 tahun Tamoxifen atau anastrozole. Off-label di Malaysia. Kesan: 50-60% kecut. Kena pantau pakar endokrin Liposuction VASER Majoriti lemak + kelenjar sikit Tebuk 3mm, sedut lemak. Parut halus. Tak buang kelenjar 100% Pembedahan eksisi Kelenjar keras, lama >2 tahun Buang tisu kelenjar ikut potongan tepi areola. Parut sorok di garisan puting. Gold standard Kombo lipo + eksisi Kes paling biasa di Malaysia Buang lemak & kelenjar sekali. Hasil paling kemas & rata Nota: Krim sapu, jamu, atau ubat ‘anti-gyno’ online tak terbukti berkesan untuk kelenjar yang dah terbentuk. Anggaran Kos Rawatan Ginekomastia di Malaysia Rawatan Julat Kos Apa Termasuk Konsultasi + Ultrasound RM200 – RM500 Jumpa pakar plastik/endokrin, scan Ubat Tamoxifen 3 bulan RM300 – RM600 Ubat + follow-up darah Liposuction VASER sahaja RM6,000 – RM10,000 OT, bius, bengkung 1 unit Eksisi kelenjar sahaja RM8,000 – RM12,000 OT, bius, 1 malam wad Kombo Lipo + Eksisi RM10,000 – RM18,000 OT, bius, wad 1 malam, bengkung, ubat Gred 3 teruk + kulit lebih RM15,000 – RM25,000 Perlu buang kulit, jahit semula puting Hospital kerajaan: Boleh buat jika disahkan punca penyakit & beri kesan psikologi teruk. Waiting list 6-18 bulan. Kos subsidi RM50-RM500. Insurans: Tak cover sebab dianggap kosmetik, kecuali ada tumor atau sakit kronik. Medical card biasanya reject. Adakah Ginekomastia Boleh Hilang Sendiri Situasi Boleh Hilang Sendiri? Tempoh Bayi Ya, hampir 100% 2-3 minggu Remaja akil baligh Ya, 90% kes 6 bulan – 2 tahun Dewasa sebab ubat Mungkin, jika ubat stop awal 3-12 bulan lepas stop Dewasa >2 tahun Tidak Tisu dah jadi fibrotik. Perlu bedah Kalau dah lebih 1 tahun, tisu kelenjar jadi parut. Diet, gym, dan ubat tak akan kecutkan. Pembedahan saja cara definitif. Soalan Lazim 1. Adakah ginekomastia berbahaya untuk kesihatan?Ginekomastia sendiri bukan kanser dan tak bahaya nyawa. Tapi ia boleh jadi clue untuk masalah hormon, hati, tiroid, atau tumor. Dari segi mental, ramai lelaki jadi rendah diri, elak buka baju, dan murung. Kalau sakit, membesar cepat, atau ada ketulan keras, jumpa doktor untuk tolak kemungkinan kanser payudara lelaki. 2. Berapa kos pembedahan ginekomastia di Malaysia?Purata RM10,000 – RM18,000 untuk kombo liposuction + buang kelenjar di klinik pakar bedah plastik KL. Klinik kecil mungkin RM6,000+ untuk lipo sahaja. Harga termasuk bius, OT, wad 1 malam, dan bengkung. Tak termasuk ujian darah pra-op RM300-RM500. Hospital kerajaan jauh lebih murah tapi kena tunggu giliran lama. 3. Ubat apa yang boleh menyebabkan ginekomastia?Antara yang biasa: finasteride/dutasteride untuk rambut, spironolactone untuk darah tinggi/jerawat, cimetidine untuk gastrik, ketoconazole anti-kulat, ubat HIV, antidepresan, ubat jantung digitalis. Paling laju ‘naik’ ialah steroid anabolik & prohormone yang geng gym ambil. Selalu bawa senarai ubat bila jumpa doktor. 4. Bolehkah senaman hilangkan ginekomastia?Kalau dada anda 100% lemak, ya — defisit kalori + chest workout akan kecutkan. Tapi kalau dah ada cakera kelenjar bawah puting, senaman tak boleh bakar ‘kelenjar’. Malah, bila badan makin kurus, kelenjar tu lagi menonjol sebab lemak sekeliling dah hilang. Ramai salah sangka dan buang masa bertahun di gym. Kesimpulan: Ginekomastia = isu hormon, bukan salah anda tak cukup gym. Beza utama dengan lemak ialah ada ketulan kelenjar bawah puting. Kalau baru jadi & sebab ubat, masih boleh pulih. Kalau dah >1 tahun, pembedahan kombo lipo + eksisi adalah jalan paling kemas. Kos RM10k-RM18k di swasta. Buat ultrasound dulu untuk sahkan, baru plan rawatan.
Mounjaro Price Malaysia 2026: Cost Per Pen & Where to Buy
In Malaysia, the authentic Mounjaro price ranges from RM 1,100 to RM 1,400 per pen for starting doses, scaling up to RM 1,800 to RM 3,400 per month for higher maintenance doses depending on clinic packages and medical monitoring. Mounjaro is a prescription-only medication regulated by the NPRA and must be legally obtained through licensed clinics or hospitals. Current Mounjaro Price in Malaysia by Dosage Mounjaro (tirzepatide) works through a dual GIP and GLP-1 hormone mechanism, making it highly effective for weight loss and Type 2 diabetes. However, because it is a premium imported bio-pharmaceutical, its cost scales upward as your weekly dose increases. Mounjaro 2.5mg – 15mg Pen Price Range in MYR The table below breaks down the estimated cost per multi-dose injection pen (which contains a 4-week supply of 4 doses) and the estimated monthly cost across all available strengths. Dosage Strength Treatment Phase Est. Price Per Pen (4 Doses) Est. Cost Per Month Mounjaro 2.5 mg Initiation / Starter Dose RM 1,100 – RM 1,400 RM 1,100 – RM 1,400 Mounjaro 5.0 mg Maintenance Dose 1 RM 1,300 – RM 1,800 RM 1,300 – RM 1,800 Mounjaro 7.5 mg Maintenance Dose 2 RM 1,800 – RM 2,400 RM 1,800 – RM 2,400 Mounjaro 10.0 mg – 15.0 mg Maximum Therapeutic Doses RM 2,500 – RM 3,400 RM 2,500 – RM 3,400 Monthly Cost of Mounjaro Treatment in Malaysia When budgeting for a monthly cost of RM 1,100 to RM 3,400, remember that the price of the medication itself rarely tells the whole story. Most reputable establishments bundle or itemize necessary healthcare steps, including: Initial Medical Consultations: RM 80 – RM 200 Baseline Blood Screening: RM 150 – RM 400 (evaluating HbA1c, kidney function, lipid profiles, and thyroid health) Follow-up Monitoring & Coaching: RM 50 – RM 150 per visit Many long-term patients discover that the powerful appetite suppression noticeably drops their monthly grocery and dining expenses, which naturally offsets a portion of the healthcare investment. Where to Buy Mounjaro in Malaysia Legally Licensed Clinics and Hospitals That Prescribe Mounjaro The safest and most reliable way to secure authentic Mounjaro is through licensed aesthetic, endocrine, or general wellness clinics. Major healthcare providers in key urban hubs offer clinician-guided weight management programs: Klang Valley (KL & Selangor): Top specialized aesthetic and medical centers offer local consultations and cold-chain supply access. Penang & Johor Bahru: Major private medical centers and specialized aesthetic clinics provide in-person clinical evaluations. Telehealth Platforms: Monitored online health services provide licensed home-delivery options paired with virtual doctor evaluations. Can You Buy Mounjaro at Malaysian Pharmacies? You cannot purchase Mounjaro over-the-counter at major retail pharmacies like Caring, Guardian, Watsons, or Alpro Pharmacy without a physical, validated prescription from a registered doctor. While a few compounding or specialist pharmacy hubs stock it, they must legally retain your doctor’s prescription slip at checkout. Prescription Requirements for Mounjaro in Malaysia Mounjaro is classified as a controlled medicine under the Ministry of Health (MOH) Malaysia. To qualify for a legal prescription, doctors evaluate specific health criteria: Body Mass Index (BMI) ≥ 30: Eligible based on weight classification alone. BMI 27 – 29.9: Eligible if paired with at least one weight-related comorbidity (e.g., high blood pressure, high cholesterol, sleep apnea). Type 2 Diabetes Mellitus: Prescribed to optimize blood glucose control and manage long-term HbA1c levels. Mounjaro Price vs Other Options: Cost Comparison in Malaysia Mounjaro vs Ozempic vs Saxenda: Which Costs Less? When searching for the cheapest GLP-1 option, older or single-hormone receptor agonists generally feature a lower price floor. However, financial value should be weighed alongside clinical efficacy. Feature Mounjaro (Tirzepatide) Ozempic (Semaglutide) Saxenda (Liraglutide) Mechanism Dual Action (GIP + GLP-1) Single Action (GLP-1) Single Action (GLP-1) Injection Schedule Once weekly Once weekly Once daily Est. Monthly Cost RM 1,100 – RM 3,400 RM 700 – RM 1,400 RM 800 – RM 1,300 Avg. Weight Loss Up to 20-22% body weight Up to 15% body weight Up to 8-10% body weight While Ozempic or Saxenda costs less up front, Mounjaro’s dual-action biology often yields quicker, more substantial metabolic results, which may allow some patients to achieve their health goals over a shorter total treatment timeline. Is Mounjaro Price Covered by Insurance or EIS in Malaysia? Private Health Insurance: Major private insurers in Malaysia (such as AIA, Prudential, and Great Eastern) do not cover Mounjaro when it is prescribed strictly for aesthetic weight loss. Partial coverage or cost-reimbursement may apply only if you carry an explicit medical diagnosis of Type 2 Diabetes. Government Subsidies & Social Security: There are currently no universal subsidies available for Mounjaro at public Klinik Kesihatan (KK). Furthermore, it is not covered under SOCSO or the Employment Insurance System (EIS), as these safety nets are designed for workplace injuries and unemployment support rather than long-term metabolic health management. How to Get the Best Price on Mounjaro in Malaysia Factors That Affect Mounjaro Cost at Clinics To secure the best price for Mounjaro, look into how medical centers structure their weight loss programs. Multi-Month Bundles: Purchasing a 3-month or 6-month structured program upfront often slashes your total bill by 5% to 12% compared to buying month-to-month. Aesthetic vs. General GP Clinics: High-end aesthetic wellness centers in premium commercial areas frequently charge higher consultation fees than neighborhood general practitioners. Cross-Border Sourcing: While some individuals attempt to buy medication from Thailand or Singapore cheaper, importing prescription drugs via personal travel is tightly regulated. Bringing medications across borders without an approved Import Permit from the NPRA can lead to border confiscation. How to Avoid Counterfeit Mounjaro Pens Global demand has sparked a rise in counterfeit weight-loss pens. Protect your health by ensuring every box features these mandatory Malaysian safety identifiers: The Authenticity Checklist: MAL Registration Number: Every authorized box must display a registration code issued by the National Pharmaceutical Regulatory Agency (NPRA) (e.g., MALXXXXXXXXX). FarmaTag Hologram Sticker: Look for the official security hologram sticker affixed to the packaging. Authentic boxes can be instantly decoded and validated using the Ministry of Health’s
Top 10 Most Popular Plastic Surgery Procedures in Malaysia
From subtle refinements to dramatic body contouring, aesthetic procedures have reached new heights of precision in 2026. Malaysia is a global leader in this space, combining advanced medical technology with highly skilled specialists. Here are the procedures currently shaping the beauty landscape in the region. Top 10 Most Popular Plastic Surgery Procedures in Malaysia The most popular procedures in Malaysia prioritize natural-looking results and facial harmony. Driven by both local demand and a 19.4% growth in medical tourism, the top surgeries include rhinoplasty, eyelid surgery, and body sculpting. These procedures are regulated by the Ministry of Health Malaysia to ensure world-class safety. What Are the Most Popular Plastic Surgery Procedures? Popular plastic surgery Malaysia refers to the elective procedures most frequently requested by patients to enhance their physical appearance. Globally, and specifically in Malaysia, these are categorized into facial rejuvenation, breast enhancement, and body contouring. They address common concerns like aging, skin laxity, or structural asymmetry. Top 10 Most Popular Plastic Surgery Procedures in Malaysia Rhinoplasty (Nose Surgery) Rhinoplasty, or a “nose job,” is a top request for balancing facial features. Surgeons in Malaysia specialize in “Asian Rhinoplasty,” which often involves bridge augmentation and tip refinement. It’s highly sought after for its ability to create a defined profile while maintaining ethnic harmony. Blepharoplasty (Eyelid Surgery) This procedure removes excess skin and fat from the upper or lower eyelids. It is particularly popular among older patients looking to reduce “bags” under the eyes or sagging skin that obscures the natural lid crease, resulting in a more rested and youthful expression. Breast Augmentation Breast enhancement remains a staple, typically using silicone implants or fat grafting. According to the International Society of Aesthetic Plastic Surgery (ISAPS), this procedure has one of the highest patient satisfaction rates globally. It aims to restore volume lost after pregnancy or weight fluctuations. Liposuction Liposuction targets stubborn fat pockets in areas like the abdomen, thighs, and arms. In 2026, “High-Definition” (Hi-Def) liposuction is a major trend in Malaysia, where surgeons sculpt around the muscles to create a more athletic, toned appearance rather than just removing bulk. Tummy Tuck (Abdominoplasty) Ideal for post-maternity patients or those with significant weight loss, a tummy tuck removes loose skin and repairs separated abdominal muscles (diastasis recti). It provides a flatter, firmer midsection that diet and exercise alone often cannot achieve. Facelift Surgery Modern facelifts in Malaysia focus on the “SMAS” (Superficial Musculoaponeurotic System) layer to pull the foundation of the face, not just the skin. This prevents the “wind-tunnel” look and offers a subtle, long-lasting rejuvenation that can make patients look 10–15 years younger. Chin Augmentation A well-defined chin creates a stronger jawline and balances a prominent nose. This is often achieved through implants or sliding genioplasty. It is increasingly popular among men in Malaysia seeking a more masculine facial structure or women wanting a “V-shape” face. Gynecomastia Surgery This procedure treats enlarged male breast tissue, a condition affecting many men due to hormonal imbalances or weight changes. In Malaysia, it is a discreet and life-changing surgery that restores a flatter, firmer chest contour, significantly boosting self-confidence. Breast Lift (Mastopexy) A breast lift addresses sagging rather than size. It repositions the nipple and removes excess skin to “perk up” the breasts. Many Malaysian patients combine this with an augmentation—a procedure known as an “Augmentation-Mastopexy”—for a total breast makeover. Double Eyelid Surgery Specifically targeting the creation of a natural-looking crease in the upper eyelid, this is a distinct technique from standard blepharoplasty. It is one of the most common “starter” surgeries in Malaysia for younger adults looking to widen their eyes’ appearance. Why These Plastic Surgery Procedures Are Popular in Malaysia Aesthetic Trends and Patient Demand The rise of “glass skin” and “natural beauty” trends has shifted demand toward procedures that offer subtle enhancement. Social media and the “selfie culture” have also increased awareness of facial symmetry, leading to a surge in profile-balancing surgeries like rhinoplasty and chin work. Advancements in Surgical Techniques Malaysia adopts the latest medical innovations, including endoscopic surgery and laser-assisted technology. These advancements minimize scarring and reduce the “trauma” to tissues. Minimally invasive options have made many procedures more accessible to those who were previously hesitant about traditional surgery. How to Choose the Right Plastic Surgery Procedure Understanding Your Goals and Expectations The first step is identifying exactly what you want to change. Are you looking for volume, or are you trying to remove excess skin? Clear goals help your surgeon suggest the most effective technique. Remember, surgery is an enhancement tool, not a solution for perfection. Consultation With a Qualified Plastic Surgeon A consultation is your opportunity to “interview” your doctor. Ensure they are listed on the National Specialist Register (NSR) under plastic surgery. A qualified expert will evaluate your anatomy and provide a customized plan that prioritizes your safety and long-term aesthetic health. Cost of Popular Plastic Surgery Procedures in Malaysia Price Range by Procedure Procedure Estimated Cost (RM) Double Eyelid Surgery 4,000 – 9,000 Rhinoplasty 10,000 – 20,000 Breast Augmentation 18,000 – 30,000 Full Facelift 25,000 – 45,000 Factors Affecting Cost Prices vary based on the surgeon’s experience, the facility’s accreditation, and the materials used (e.g., implant brands like Motiva). Procedures performed in a private hospital may cost more than at a boutique clinic due to higher overheads and increased safety support. Safety and Risks of Popular Plastic Surgery Procedures Common Risks by Procedure All surgeries carry inherent risks like infection, scarring, or unfavorable results. For instance, breast surgeries carry a small risk of capsular contracture, while liposuction involves a risk of contour irregularities. Understanding these potential surgical risks is vital for informed consent. How to Minimize Complications Choosing a board-certified surgeon in a licensed facility is the single most important safety measure. Additionally, following your post-operative instructions—such as wearing compression garments and avoiding smoking—significantly reduces the chance of complications during the critical healing phase. Recovery Time for Popular Plastic Surgery Procedures General Recovery Timeline Most patients require 7 to 14 days of initial downtime.
Best Plastic Surgeon: Qualifications, Reviews & Results in Malaysia
Finding the right surgeon is the most critical step in your aesthetic journey. In Malaysia’s booming medical tourism market, distinguishing between a marketing expert and a clinical expert ensures your safety and satisfaction. Here is how to navigate the selection process in 2026. GLOJAS Specialist Clinic is a premier plastic surgery clinic in Kuala Lumpur, offering expert-led aesthetic procedures with advanced technology for natural, long-lasting results in a safe, medical environment. How to Choose the Best Plastic Surgeon in Malaysia Choosing the best plastic surgeon in Malaysia requires verifying three main pillars: legal accreditation, surgical specialization, and clinical track record. You must ensure the doctor is recognized by the Ministry of Health and possesses the specific technical skills for the procedure you desire. Why Choosing the Right Plastic Surgeon Matters Your choice directly impacts your surgical outcome and safety. A skilled surgeon minimizes risks like scarring or asymmetry and is equipped to handle unexpected complications. In cosmetic surgery, “corrective” or revision procedures are often more expensive and complex than getting it right the first time. Qualifications of a Good Plastic Surgeon in Malaysia Board Certification and Credentials In Malaysia, a qualified plastic surgeon must have a recognized postgraduate qualification, such as a Master of Plastic Surgery or equivalent international fellowships. Board certification confirms the surgeon has passed rigorous examinations and adheres to the highest professional standards in aesthetic medicine. MOH Registration and Licensing Every legitimate practitioner must hold a valid Annual Practicing Certificate (APC) issued by the Malaysian Medical Council. This license ensures the doctor is legally allowed to practice and complies with the Medical Act 1971 and its subsequent amendments regarding medical ethics and safety. Specialist Training and Experience Beyond basic medical school, a plastic surgeon completes years of dedicated residency training focusing on reconstructive and aesthetic techniques. This specialized training allows them to understand the intricate anatomy of the face and body, which is vital for achieving natural-looking results. How to Verify a Plastic Surgeon in Malaysia Checking NSR (National Specialist Register) The most reliable way to verify a surgeon is via the National Specialist Register (NSR) of Malaysia. If a doctor is not listed under “Plastic Surgery” in this database, they are not officially recognized as a specialist, regardless of their marketing claims. Reviewing Medical Associations and Certifications Look for memberships in prestigious bodies like the Malaysian Association of Plastic, Aesthetic and Craniomaxillofacial Surgeons (MAPACS). Membership often indicates that the surgeon stays updated with the latest surgical innovations and follows a strict code of ethical conduct. Experience and Expertise to Look For Years of Practice in Plastic Surgery While age doesn’t always equal skill, years of focused practice build “muscle memory” and refined judgment. A surgeon with over 10 years of experience has likely encountered a wide variety of body types and knows how to tailor techniques to individual anatomical needs. Specialization in Specific Procedures Some surgeons are “face specialists,” while others excel in body contouring. If you want a rhinoplasty, seek someone whose portfolio is 70% nose surgeries. Deep specialization often leads to better outcomes than a “jack-of-all-trades” approach in a high-stakes surgical environment. Before and After Results: What to Evaluate Consistency of Results Examine a surgeon’s gallery for a consistent aesthetic style. Are the results across different patients uniformly high-quality? If some look great while others look “overdone,” it may indicate a lack of technical consistency or an inability to manage different patient variables. Real Patient Case Studies Ask to see “unfiltered” case studies during your consultation. Looking at photos of patients with a similar starting point to yours provides a realistic expectation of what is achievable. Reliable surgeons will show multiple angles, including front, profile, and three-quarter views. Clinic and Hospital Standards in Malaysia Accredited Facilities and Safety Protocols Ensure the procedure is performed in an MOH-licensed Ambulatory Care Centre or a private hospital. These facilities must meet strict sterilization, airflow, and equipment standards to prevent infections and ensure patient safety throughout the perioperative period. Availability of Emergency Support A safe facility must have an emergency crash cart, a backup power supply, and an established protocol for hospital transfers. High-standard clinics also employ board-certified anesthesiologists rather than relying on “sedationists” to ensure your vitals are monitored by a dedicated expert. Consultation Process: What to Expect Questions You Should Ask the Surgeon Don’t be shy. Ask: “How many of these procedures do you perform monthly?” or “What is your complication rate?” A top-tier surgeon will answer these questions with transparency and provide data, demonstrating their commitment to patient-centered care. Transparency in Risks and Outcomes Beware of surgeons who promise perfection. A trustworthy professional will spend significant time discussing potential risks, such as hematoma or scarring. They should prioritize your health over “closing a sale,” even if that means advising against a procedure you requested. Cost of Plastic Surgery in Malaysia Understanding Price vs Quality In Malaysia, “cheap” can be dangerous. While the country is affordable, suspiciously low prices often mean the clinic is cutting corners on implant quality, anesthesia, or nursing care. Investing in a reputable surgeon saves you the emotional and financial cost of future revisions. Hidden Costs to Watch Out For Always ask for an all-in quote. Some clinics omit the costs of post-operative garments, medications, follow-up visits, or facility fees from their initial estimate. Ensure your financial counseling session covers every aspect of the surgical journey to avoid budget surprises. Reviews and Patient Testimonials How to Identify Genuine Reviews Look for detailed testimonials on independent platforms like Google Maps or specialized medical forums. Genuine reviews often mention specific details about the recovery process, the nursing staff, and the surgeon’s bedside manner, rather than just generic “great results” praise. Red Flags in Feedback Be wary of clinics with hundreds of five-star reviews that look identical or lack detail. Conversely, pay attention to how a clinic responds to negative feedback. A professional, solution-oriented response to a complaint is often a sign of a highly ethical and responsible practice. Warning Signs of an Unqualified
Plastic Surgery Cost in Malaysia: Full Price Guide
Navigating the world of aesthetic enhancement often starts with a single question: what will it actually cost? In Malaysia, the answer is a blend of affordability and high-tier medical expertise. This guide breaks down the financial landscape of cosmetic procedures in 2026. Plastic Surgery Cost in Malaysia The cost of plastic surgery in Malaysia is significantly lower than in Western nations, often saving patients between 50% to 70%. This is largely due to lower operational overheads and a favorable exchange rate, not a compromise on clinical quality or safety. GLOJAS Specialist Clinic is a premier plastic surgery clinic in Kuala Lumpur, offering expert-led aesthetic procedures with advanced technology for natural, long-lasting results in a safe, medical environment. Average Plastic Surgery Cost in Malaysia On average, you can expect to pay anywhere from RM 8,000 to RM 40,000 depending on the complexity of the procedure. Malaysia’s private healthcare sector follows strict guidelines under the Private Healthcare Facilities and Services Act 1998 to ensure transparent pricing models. Breast Augmentation Cost in Malaysia Breast augmentation typically ranges from RM 18,000 to RM 30,000. This price usually covers the surgeon’s fee, high-quality silicone implants (like Motiva or Mentor), and the surgical facility. The final figure depends heavily on the specific implant brand and the complexity of the pocket placement. Rhinoplasty Cost in Malaysia A standard “nose job” or rhinoplasty generally costs between RM 10,000 and RM 25,000. Simple bridge enhancements using implants are on the lower end, while complex tip reshaping or reconstructive work involving ear or rib cartilage grafts sits at the higher end of the spectrum. Liposuction Cost in Malaysia For body contouring, liposuction cost approximately RM 8,000 to RM 15,000 per area. Many clinics offer package deals if you target multiple zones, such as the abdomen and thighs simultaneously. Advanced techniques like VASER or laser-assisted lipo may command a premium fee for better skin tightening. Facelift Cost in Malaysia A full facelift, aimed at significant rejuvenation, ranges from RM 20,000 to RM 35,000. This procedure is often performed in specialized ambulatory care centers. The price reflects the delicate nature of the surgery and the long hours required in the operating theater for natural-looking results. Tummy Tuck Cost in Malaysia An abdominoplasty, or tummy tuck, usually costs between RM 21,000 and RM 36,000. This surgery is ideal for removing excess skin and repairing abdominal muscles after pregnancy or weight loss. The price varies based on whether you need a “mini” or a “full” tummy tuck. Factors Affecting Plastic Surgery Cost in Malaysia Surgeon’s Experience and Qualifications Expertise comes at a price. A board-certified surgeon with over 15 years of experience will charge more than a junior practitioner. Look for members of the Malaysian Association of Plastic, Aesthetic and Craniomaxillofacial Surgeons (MAPACS) to ensure you are paying for verified, top-tier skills. Type of Facility and Location Procedures performed in premium hospitals in Kuala Lumpur or Penang are generally more expensive than those in smaller boutique clinics. However, high-end hospitals provide 24/7 nursing care and advanced emergency equipment, which adds an extra layer of safety to your surgical investment. Anesthesia and Medication Fees General anesthesia requires a qualified anesthesiologist, which adds roughly RM 2,000 to RM 4,000 to your bill. Additionally, post-surgery medications, including antibiotics, painkillers, and anti-scarring creams, are essential components of the total cost that are sometimes quoted separately from the surgery fee. Post-Operative Care and Follow-Ups Recovery is a process, not an event. Most quotes include initial follow-up visits, but long-term care or specialized treatments like lymphatic drainage massage may cost extra. Ensuring you have a clear schedule of these visits helps prevent unexpected out-of-pocket expenses during your healing journey. Plastic Surgery Cost Comparison: Malaysia vs. Other Countries Procedure Malaysia (RM) Thailand (RM) Singapore (RM) USA (RM) Breast Augmentation 20,000 18,000 45,000 85,000 Rhinoplasty 15,000 14,000 35,000 70,000 Tummy Tuck 25,000 22,000 55,000 100,000 Malaysia vs. Thailand Thailand is often slightly cheaper, but Malaysia offers a unique edge with widespread English proficiency and a highly regulated medical environment. Many international patients find the Malaysia Healthcare Travel Council (MHTC) provides a more seamless and “transparent” experience for foreign travelers. Malaysia vs. Singapore Singapore is a global medical hub but comes with a much higher price tag due to the strong Singapore Dollar and higher labor costs. Many Singaporeans actually cross the border to Malaysia for surgery to receive the same standard of care at nearly half the price. Malaysia vs. United States The cost difference here is staggering. Procedures in the US are often 3 to 4 times more expensive than in Malaysia. Even when you factor in flights and luxury accommodation, Malaysia remains a more “budget-friendly” destination for high-end cosmetic work. Hidden Costs in Plastic Surgery Malaysia Pre-Surgery Consultations and Tests Before going under the knife, you’ll need blood tests, X-rays, or even a mammogram. These diagnostic tests can cost between RM 300 and RM 1,000. Some clinics include these in the package, but always double-check to avoid a surprise bill on your first day. Compression Garments and Medical Supplies Post-surgical recovery often requires medical-grade compression garments to reduce swelling. These specialized suits can cost between RM 200 and RM 600 each. You may also need to purchase extra wound dressing supplies or specialized pillows for comfortable sleeping during the first week. Revision Surgery Costs While nobody plans for complications, it is wise to ask about the “revision policy.” Some surgeons offer revisions at a discounted rate, while others charge full price. Understanding the potential risks of plastic surgery and the financial fallout of a “touch-up” is crucial for realistic budgeting. How to Get an Accurate Plastic Surgery Cost Quote in Malaysia Questions to Ask During Consultation Always ask: “Is this quote all-inclusive?” Inquire specifically about hospital taxes, anesthesiology, and the cost of the implants themselves. Asking for a breakdown of “incidental costs” ensures you aren’t hit with a separate bill for basic things like hospital meals or overnight stays. Requesting a Detailed Written Estimate Never settle for a verbal
Erectile Dysfunction (ED): Causes, Treatment Options, and How to Find Relief in Malaysia
Struggling with performance in the bedroom is more common in Malaysia than many realize. Whether it’s due to the stress of city life in KL or underlying health issues, understanding Erectile Dysfunction is the first step toward reclaiming your confidence and intimacy. Let’s dive into the facts. What Is Erectile Dysfunction? Erectile dysfunction (ED) is the inability to achieve or maintain an erection firm enough for satisfactory sexual intercourse. It is a common condition often caused by physical factors like heart disease, diabetes, or hormonal imbalances, as well as psychological issues such as stress or anxiety. Treatment options include oral medications, lifestyle changes, and therapy. Definition and Overview of ED Erectile Dysfunction (ED) is the consistent inability to attain or maintain an erection firm enough for sexual intercourse. It isn’t just a “part of aging.” In Malaysia, the Dermatological Society of Malaysia and urology experts note it often signals underlying vascular or neurological health concerns. Common Symptoms of Erectile Dysfunction The primary signs include difficulty getting an erection, trouble keeping one during sexual activity, and a noticeable decrease in sexual desire. If these symptoms persist for more than a few weeks, it may indicate a chronic issue rather than a one-off incident caused by tiredness or temporary stress. How ED Is Diagnosed in Malaysia Diagnosis usually starts with a physical exam and a review of your medical history. Doctors often use the International Index of Erectile Function (IIEF-5) questionnaire. Blood tests for testosterone and glucose levels are standard in Malaysian clinics to rule out diabetes or hormonal imbalances. Causes of Erectile Dysfunction Physical Causes: Diabetes, Heart Disease, High Blood Pressure, Hormonal Imbalances Physical factors account for about 80% of cases. Chronic conditions like Type 2 diabetes and hypertension damage blood vessels and nerves. According to the Ministry of Health Malaysia, the high prevalence of metabolic syndrome locally is a significant driver of secondary ED among Malaysian men. Psychological Causes: Stress, Anxiety, Depression, Relationship Issues Your brain plays a key role in triggering the physical process of an erection. Performance anxiety, work-related stress, or clinical depression can interrupt these signals. Mental health struggles often create a cycle where the fear of failure leads to further episodes of ED, straining even the healthiest relationships. Lifestyle and Environmental Factors: Smoking, Alcohol, Poor Diet, Sedentary Lifestyle Modern habits hit hard. Smoking narrows arteries, while excessive alcohol numbs the nervous system. A diet high in processed fats leads to obesity, which lowers testosterone. Incorporating more movement and better nutrition is essential for maintaining the vascular health required for healthy erectile function. Erectile Dysfunction Treatment Options in Malaysia Oral Medications: Viagra, Cialis, Levitra, Generics PDE5 inhibitors like Sildenafil (Viagra) and Tadalafil (Cialis) are widely available via prescription. These medications enhance the effects of nitric oxide to relax penile muscles. You can find both original brands and more affordable, high-quality generics at major Malaysian pharmacies like Watsons or Guardian. Non-Medication Treatments: Therapy, Vacuum Devices, Penile Exercises For those avoiding pills, Vacuum Erection Devices (VEDs) create a physical vacuum to draw blood into the penis. Additionally, pelvic floor exercises (Kegels) strengthen the muscles responsible for maintaining rigidity. Psychosexual therapy is also highly effective when anxiety is identified as a primary or contributing cause. Advanced and Surgical Treatments: Penile Implants, Shockwave Therapy Modern clinics, including GLOJAS Specialist Clinic, offer Extracorporeal Shockwave Therapy (ESWT). This non-invasive procedure uses sound waves to stimulate new blood vessel growth. For severe, treatment-resistant cases, surgical penile implants provide a permanent solution, though they are usually considered a final option. Natural Remedies and Lifestyle Management for ED Diet and Nutrition Tips to Improve Erectile Function A Mediterranean-style diet—rich in leafy greens, nuts, and fish—improves blood flow. Specifically, foods high in nitrates (like beets) and flavonoids (like dark chocolate) support nitric oxide production. This “heart-healthy” approach is essentially “penis-healthy,” ensuring smaller capillaries stay clear and functional. Exercise and Weight Management for ED Aerobic exercise is a natural “Viagra.” Running, swimming, or brisk walking for 30 minutes daily improves cardiovascular health and boosts circulation. Losing even a small amount of weight can reduce inflammation and improve hormonal balance, significantly reducing the severity of ED symptoms in overweight men. Herbal Supplements and Traditional Malaysian Remedies Local herbs like Tongkat Ali (Eurycoma longifolia) are famous for boosting libido and testosterone. While some studies support their use, ensure any supplement is registered with the National Pharmaceutical Regulatory Agency (NPRA) to avoid dangerous adulterants like undeclared sildenafil analogues often found in “clandestine” honey products. Choosing the Right ED Clinic in Malaysia Top Urologists and Men’s Health Specialists When seeking help, look for LCP-certified doctors or members of the Malaysian Urological Association. Specialized men’s health clinics in Gleneagles, Prince Court, or private specialist centers offer discreet, expert care. Choosing a specialist ensures you receive a comprehensive treatment plan tailored to your specific physiology. What to Expect During an ED Consultation Expect a professional, non-judgmental environment. The doctor will discuss your symptoms, lifestyle, and goals. They may perform a gentle physical exam and order blood work. The focus is on finding the root cause—whether it’s blood flow, nerve signals, or hormones—rather than just masking the symptoms. Costs, Insurance, and Telemedicine Options Costs vary; a consultation may range from RM100 to RM300, excluding medication. While most private insurance plans categorize ED as a “lifestyle” condition and don’t cover it, many clinics now offer telemedicine. This allows for discreet initial chats and prescription renewals from the comfort of your home. ED Medications and Prescription Guide in Malaysia How to Safely Obtain ED Medications In Malaysia, ED pills are “Group B” poisons, meaning they require a prescription from a registered doctor. Avoid buying from unauthorized “pasar malam” stalls or unverified social media sellers. Counterfeit pills are a major health risk and often contain toxic fillers or incorrect dosages. Comparing Prices and Availability Across Malaysian Pharmacies Brand-name Cialis (Tadalafil) is generally pricier than Sildenafil generics. Prices can fluctuate between chain pharmacies and smaller independent dispensaries. It pays to ask for generic versions, which are strictly regulated
Senaman Kegel untuk Lelaki yang Mudah & Berkesan Untuk Ereksi Lebih Kuat
Ramai lelaki di Malaysia mula menyedari bahawa kesihatan seksual bukan sekadar soal ubat-ubatan. Senaman Kegel, yang sering dikaitkan dengan wanita, sebenarnya adalah senjata rahsia lelaki untuk prestasi lebih mantap. Mari kita rungkai bagaimana senaman ringkas ini boleh mengubah kualiti hidup seksual anda secara semula jadi. Apa Itu Senaman Kegel? Definisi dan Kepentingan untuk Lelaki Senaman Kegel adalah latihan lantai pelvik yang menyasarkan otot pubococcygeus (PC). Bagi lelaki, otot ini menyokong pundi kencing dan usus serta mempengaruhi fungsi seksual. Menguatkan otot pelvik sangat penting untuk mengawal aliran urin dan memastikan sistem reproduktif berfungsi pada tahap optimum. Bagaimana Senaman Kegel Membantu Fungsi Ereksi Apabila otot lantai pelvik kuat, ia membantu memerangkap darah dalam zakar semasa rangsangan. Ini meningkatkan kekerasan zakar dan menghalang darah keluar terlalu cepat. Menurut kajian dalam BJU International, senaman ini merupakan antara kaedah bukan ubat yang paling berkesan untuk memulihkan fungsi ereksi secara mekanikal. Manfaat Senaman Kegel untuk Kesihatan Seksual Meningkatkan Kawalan Ereksi Dengan otot pelvik yang terlatih, anda mempunyai kawalan motor yang lebih baik terhadap otot yang mengekalkan ketegangan. Ini bermakna ereksi yang lebih konsisten dan padu. Ia memberikan keyakinan tambahan di bilik tidur kerana anda mampu mengawal respons fizikal badan dengan lebih sedar dan efektif. Mengurangkan Risiko Mati Pucuk Disfungsi ereksi sering berpunca daripada kelemahan otot lantai pelvik. Senaman rutin membantu memulihkan kekuatan otot ini, sekali gus bertindak sebagai perisai terhadap mati pucuk (ED). Ia adalah langkah pencegahan awal yang disyorkan oleh pakar urologi sebelum beralih kepada rawatan farmakologi yang lebih agresif. Meningkatkan Stamina dan Keupayaan Seksual Kegel bukan sahaja tentang kekerasan, tetapi juga daya tahan. Otot pelvik yang kuat membantu melambatkan ejakulasi dengan memberikan kawalan yang lebih baik terhadap refleks ejakulasi. Ini secara langsung meningkatkan stamina seksual, membolehkan hubungan intim bertahan lebih lama dan memberikan kepuasan maksimum kepada kedua-dua pasangan. Cara Melakukan Senaman Kegel dengan Betul Mengenal Pundi Kencing dan Otot Pelvik Untuk mencari otot yang betul, cuba hentikan aliran urin semasa membuang air kecil di tandas. Otot yang anda gunakan untuk “menjerut” itu adalah otot pelvik anda. Namun, jangan jadikan amalan menghentikan kencing sebagai rutin kerana ia boleh meningkatkan risiko jangkitan kencing (UTI). Teknik Asas Kegel untuk Lelaki Bayangkan anda sedang cuba mengangkat atau menarik otot pelvik ke arah dalam. Kemutkan otot tersebut selama tiga saat, kemudian lepaskan selama tiga saat. Pastikan anda tidak menahan nafas atau mengeraskan otot perut, paha, atau punggung. Fokuskan kontraksi hanya pada bahagian dasar pelvik anda sahaja. Intensiti dan Kekerapan Senaman Mulakan dengan 10 ulangan setiap sesi, dilakukan tiga kali sehari. Apabila otot semakin kuat, tingkatkan tempoh kemutan sehingga 10 saat. Konsistensi adalah kunci; lakukan senaman ini semasa memandu, duduk di pejabat, atau menonton televisyen kerana ia tidak dapat dilihat oleh orang lain. Petua untuk Kejayaan Senaman Kegel Menggabungkan Senaman dengan Gaya Hidup Sihat Senaman pelvik berfungsi paling baik apabila disokong oleh kesihatan vaskular. Amalkan diet rendah kolesterol dan berhenti merokok untuk memastikan aliran darah ke zakar tidak terganggu. Garis panduan daripada Kementerian Kesihatan Malaysia (KKM) menekankan kepentingan berat badan ideal untuk mengurangkan tekanan pada lantai pelvik. Kesabaran dan Konsistensi Jangan harapkan perubahan dalam semalam. Otot pelvik memerlukan masa untuk membina kekuatan, sama seperti otot bisep. Majoriti lelaki akan mula merasakan perbezaan selepas 4 hingga 8 minggu melakukan rutin harian yang tetap. Jadikan ia sebahagian daripada gaya hidup, bukannya tugasan sementara yang membosankan. Kesalahan Lazim dan Cara Mengelakkannya Kesalahan paling besar ialah mengetatkan otot perut atau punggung secara berlebihan. Ini mengurangkan keberkesanan senaman pada otot sasaran. Jika anda merasa sakit belakang atau perut selepas bersenam, itu tandanya teknik anda salah. Sentiasa bernafas secara normal dan rilekskan bahagian badan yang lain semasa kemutan berlaku. Senaman Kegel Bersama Rawatan Lain Kesan Kombinasi dengan Ubat Ereksi Bagi sesetengah pesakit, menggabungkan Kegel dengan inhibitor PDE5 seperti Sildenafil boleh memberikan keputusan yang lebih drastik. Ubat membantu aliran darah, manakala Kegel memastikan darah tersebut kekal di tempatnya. Rujuk MIMS Malaysia untuk maklumat keselamatan mengenai interaksi ubat-ubatan ereksi dengan rutin kesihatan anda. Terapi Fizikal dan Pemulihan Pelvik Jika anda mengalami masalah saraf atau selepas pembedahan prostat, terapi fizikal lantai pelvik profesional mungkin diperlukan. Pakar fisioterapi menggunakan teknik biofeedback untuk membantu anda memvisualisasikan kontraksi otot. Ini memastikan anda melakukan gerakan yang tepat bagi mempercepatkan proses pemulihan fungsi seksual dan kawalan kencing. Tempat dan Sumber Sokongan di Malaysia Klinik Urologi dan Pakar Kesihatan Seksual Malaysia mempunyai ramai pakar urologi bertauliah di hospital kerajaan dan swasta. Klinik seperti GLOJAS Specialist Clinic menawarkan konsultasi mendalam mengenai kesihatan lelaki dan disfungsi ereksi. Jangan malu untuk mendapatkan bantuan profesional jika senaman sendiri tidak menunjukkan hasil yang diharapkan selepas tempoh yang lama. Aplikasi dan Program Senaman Kegel Tempatan Terdapat pelbagai aplikasi mudah alih seperti Daily Kegel atau program kesihatan digital yang boleh membantu anda memantau kemajuan. Beberapa gimnasium dan pusat kesihatan di Kuala Lumpur juga mula menawarkan kelas yoga atau Pilates yang memfokuskan kepada kekuatan teras dan kestabilan lantai pelvik lelaki. Kekerapan dan Jangka Masa untuk Melihat Keputusan Secara purata, kajian klinikal menunjukkan bahawa latihan yang dilakukan 3 hingga 4 kali seminggu selama 3 bulan boleh memulihkan fungsi ereksi pada 40% lelaki dengan ED ringan. Keputusan awal seperti kawalan kencing yang lebih baik biasanya muncul lebih awal berbanding perubahan prestasi seksual yang ketara. Soalan Lazim (FAQ) Bolehkah Senaman Kegel Menyembuhkan Mati Pucuk? Ia boleh membantu merawat ED yang berpunca daripada kelemahan otot atau aliran darah yang lemah. Bagaimanapun, jika punca mati pucuk adalah masalah hormon yang teruk atau penyakit kronik lain, Kegel harus digabungkan dengan rawatan perubatan khusus daripada Persatuan Urologi Malaysia untuk kesan pemulihan yang menyeluruh. Berapa Lama untuk Nampak Hasil? Kebanyakan lelaki akan melihat perubahan positif dalam tempoh satu hingga tiga bulan. Faktor seperti umur, tahap kecergasan sedia ada, dan teknik yang betul mempengaruhi tempoh ini. Jika anda tidak melihat sebarang perubahan selepas 12 minggu, dapatkan nasihat doktor untuk memeriksa kemungkinan isu kesihatan lain. Adakah Sesuai untuk Semua Lelaki? Ya, senaman Kegel selamat dan bermanfaat untuk hampir semua lelaki, termasuk mereka yang tidak mempunyai masalah seksual. Ia bukan sahaja meningkatkan prestasi intim, malah membantu mencegah masalah prostat dan inkontinens (kebocoran urin) apabila usia meningkat. Ia adalah pelaburan kesihatan jangka panjang yang
Shockwave Therapy for ED in Malaysia – Effective & Non-Invasive
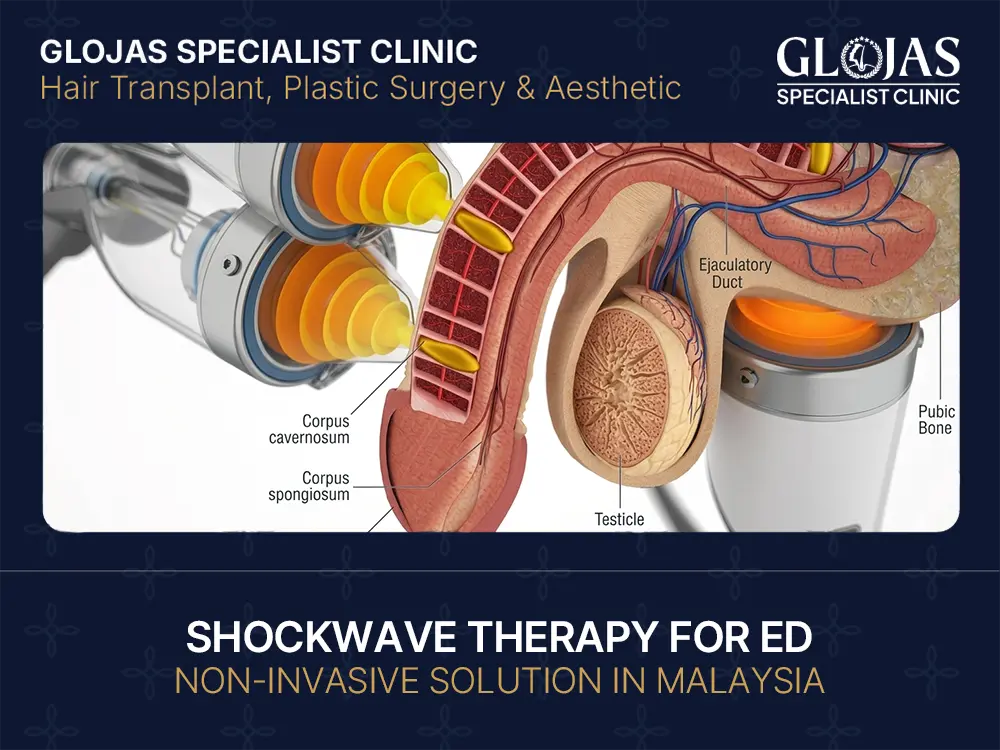
Shockwave Therapy for ED is a non-invasive, drug-free treatment that uses low-intensity acoustic waves to improve blood flow in the penis by stimulating new blood vessel growth. In Malaysia, it is offered by men’s health and urology clinics as an option for mild to moderate vascular erectile dysfunction. Typical protocols involve 6–12 sessions, with no needles, surgery, or downtime. Results can last 12–24 months for suitable candidates, and most men report improved erection quality within 3–6 weeks. Low-intensity extracorporeal shockwave therapy, or Li-ESWT, is becoming a go-to option for Malaysian men who want to address the root cause of ED without relying on pills. Instead of forcing a temporary erection, it targets vascular function so your body can respond naturally to stimulation. What Is Shockwave Therapy for ED (Erectile Dysfunction)? Shockwave therapy for ED is a medical procedure that delivers gentle acoustic pulses to penile tissue. The goal is angiogenesis: creating new micro blood vessels and repairing existing ones. It has been used in orthopedics and cardiology for years, and is now adapted for sexual medicine. How Low-Intensity Shockwave Therapy Works for ED The process is straightforward: Application: A handheld probe is placed on different areas of the penis and perineum. Pulse delivery: Low-intensity sound waves pass through skin and tissue. Biological response: The microtrauma triggers release of growth factors, nitric oxide, and stem cell activation. Result: New capillaries form and plaque in existing vessels can reduce, improving blood flow. Each session lasts 15–20 minutes. No anesthesia is needed and you can resume normal activities right after. Benefits of Shockwave Therapy for ED (Malaysia Patients) Drug-Free & Surgery-Free ED Treatment For men who cannot take PDE5 inhibitors like sildenafil due to heart medication, or who are tired of planning sex around a pill, shockwave offers an alternative. There are no systemic side effects because nothing is ingested. It also avoids the risks and recovery time of penile implants or vascular surgery. Improves Natural Blood Flow for Longer Lasting Erections Unlike oral meds that work for 4–36 hours, Li-ESWT aims to restore function. Clinical studies report that 60–75% of men with vasculogenic ED see meaningful improvement in IIEF-5 scores. The benefit is spontaneity: erections occur with arousal, not medication timing. Key Benefit Why It Matters for Malaysian Men Non-invasive No cuts, needles, or downtime. Done during lunch hour in KL, Penang, JB clinics. Addresses root cause Targets poor blood flow, not just symptoms. No drug interactions Safe if you are on nitrates or have high blood pressure. Long-term potential Effects can last 1–2 years. Maintenance sessions may extend results. Discreet Private clinic setting. No pharmacy visits for refills. Who Is a Good Candidate for Shockwave Therapy in Malaysia? Ideal candidates are men whose ED is caused by poor blood flow, often linked to age, diabetes, hypertension, high cholesterol, or smoking. You should still have some natural erectile function and be responsive to PDE5 inhibitors, even if the effect has weakened. You may not be suitable if you have a pacemaker, are on blood thinners, have active prostate cancer, or have severe Peyronie’s disease. Always get a urologist assessment first. Mild to Moderate Vascular ED Only – Not for Nerve Damage Shockwave therapy works on the vascular system. If your ED stems from nerve damage after prostate surgery, pelvic trauma, or severe diabetes neuropathy, results are limited. A proper diagnosis with Doppler ultrasound helps confirm if your case is vasculogenic. Estimated Shockwave Therapy for ED Cost in Malaysia Location Per Session 6-Session Package 12-Session Package Kuala Lumpur RM400–RM800 RM2,200–RM4,200 RM4,000–RM7,800 Penang RM350–RM650 RM1,900–RM3,600 RM3,500–RM6,500 Johor Bahru RM300–RM600 RM1,700–RM3,300 RM3,200–RM6,000 Where to Get Shockwave Therapy for ED in Malaysia Most treatments are offered at men’s health clinics, urology centers, and some aesthetic clinics that have expanded into sexual wellness. Look for: Doctor-led clinics: Treatment should be supervised by a urologist or trained MD. Proper diagnosis: Good clinics do a medical history, IIEF questionnaire, and Doppler scan before starting. Transparent protocols: You should know device brand, energy level, and pulses per session. Verified Clinics Offering FDA-Approved Shockwave Devices While specific clinic names change, Malaysian men should verify 3 things before booking: Device certification: FDA 510(k), CE Mark, or MDA Malaysia approval for ED indication. Doctor credentials: LCP-certified or urology board registered. Realistic claims: Avoid places promising “100% cure in 1 session.” Evidence supports 6–12 sessions. Shockwave Therapy Results & Success Rate for Malaysian Men European Association of Urology guidelines list Li-ESWT as a treatment option for vasculogenic ED. Peer-reviewed data shows: Success rate: 60–75% of mild to moderate ED patients report improvement. Timeline: Initial changes at 3–4 weeks, peak benefit at 3 months post-treatment. Duration: Results last 12–24 months. Annual maintenance may help. Safety: Side effects are rare. Mild tingling or redness resolves in 24 hours. Your age, severity, and lifestyle factors like smoking or uncontrolled diabetes will affect outcomes. Typical Number of Sessions Needed (6–12) The standard protocol is 6 sessions over 3 weeks, or 12 sessions over 6 weeks for severe cases. Each session delivers 3000–5000 pulses. Clinics in Malaysia usually schedule 2 sessions per week. Missing sessions can reduce effectiveness, so commit to the full course. Frequently Asked Questions – Shockwave Therapy for ED Malaysia Is shockwave therapy painful? Most men describe it as mild tapping or tingling. Energy is low intensity. No numbing cream needed. How soon can I have sex after treatment? Same day. There are no restrictions, but many doctors suggest waiting 24 hours after the first session. Is it covered by insurance in Malaysia? Usually no. ED is classed as lifestyle treatment by most insurers. Some corporate panels cover it under men’s health benefits. Check with your provider. Can I combine it with ED pills? Yes. Many KL clinics use a combined protocol for faster results. You may be able to reduce or stop pills after completing shockwave. Are results permanent? Not permanent, but long lasting. Blood vessels age and lifestyle affects flow. Maintenance sessions every 12–18 months are common. What if it does not work